
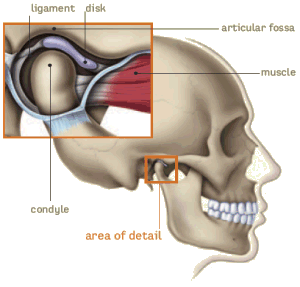
Notice the temporalis muscle that runs along your "temple" and the side of your head. Many headache sufferers report having pain in this area and frequently link it to high stress levels. This muscle not only helps to clench your jaw tight but also has blood vessels that run in close proximity to it. Due to this anatomical mapping, many people that report throbbing headaches or a dull ache in the "temple" area after a high stress situation may be experiencing a side effect of temporalis muscle spasm from jaw clenching. Incidentally, there are also a few conditions such as temporal arteritis and polymyaliga rheumatica that may effect that same area and as a result may have similar symptoms. These conditions are more often found in older individuals (over 50) that suffer from immune dysfunction such as autoimmune disorders, frequent infections, and high doses of antibiotics. Consult your doctor for more information on these conditions.
The masseter muscle is the top layer of muscle that helps to pull the jaw shut tightly. I don't frequently find any issues with this muscle as its motion is pretty straight forward and with talking and chewing daily usually gets enough motion and stretching to avoid spasm.
The second layer of muscle underneath the masseter muscle is home to two muscles, the medial and lateral pterygoids. Refer to the picture below for a better understanding of where they attach. Notice the lateral pterygoid muscle attaches at two different points on the maxilla (upper jaw) while the medial is made up on one attachment. The two pterygoid muscles work together to not only lower the jaw but also open and thrust it forward in motions necessary for chewing and talking. Because these muscles are involved in a complex motion process, I frequently find them in spasm and very tender when palpated.
The other muscle shown is the digastric muscle which aids in allowing the jaw to open by pulling the mandible downward. In high stress individuals and jaw clenchers I typically find this muscle to be tender due more to overuse rather than spasm.
So now that we've covered the anatomy a bit more let's talk about what happens in TMJ dysfunction. TMJ dysfunction can be characterized by a number of different things including generalized jaw pain and weakness to jaw tracking variants as well as clicking, popping, and grinding upon opening the jaw. Jaw pain and weakness is usually a combination of issues due to nerve involvement in addition to the mechanical dysfunction caused by muscle imbalance and spasm. Jaw tracking variants can be due to improper muscle balance of the jaw muscles due to muscle spasm. The clicking, popping, and grinding sounds are usually due to degeneration and/or injury to the disc that cushions the mandible and as a result the disc is either not allowing a smooth gliding mandibular motion or the ligaments holding the disc may be injured or torn allowing the disc to "click" during jaw motion.
The nerve involvement associated with jaw pain and weakness may be due to irritation or direct pressure on a nerve from inflammation in the TMJ or from muscle spasms in the surrounding musculature. The muscle involvement can frequently be affected by your misaligned "bite" as well as clenching. Teeth are supposed to overlap and contact at the same time in your bite, however many factors such as a history of braces or tooth extraction can cause these contact points to shift. The shifting can cause high points on the teeth so that one side or one tooth contacts first in your bite. This high point can not only put stress on that tooth (causing loose teeth and a painful gum line due to exposed nerve) but also can cause the jaw muscles to react and contract unevenly which can lead to muscle spasms.
So what can you do about it? Talk to your dentist! Many dentists are now trained in a procedure called occlusal adjustments which reshape the surface of the teeth to eliminate or lessen the high spots in your bite. In addition to your dentist, talk to other health professionals you see such as a chiropractor and/or massage therapist as they can address the muscle spasms and may be able to offer stress management techniques to help prevent teeth clenching. Some chiropractors are also trained in adjustment procedures that are gentle and specific to help realign the TMJ joint using soft tissue and Activator techniques.
So much for a "quick" blog post right???

No comments:
Post a Comment